Aerosol Therapy in Dogs & Cats
Elizabeth Rozanski, DVM, DACVECC, DACVIM, Cummings School of Veterinary Medicine at Tufts University
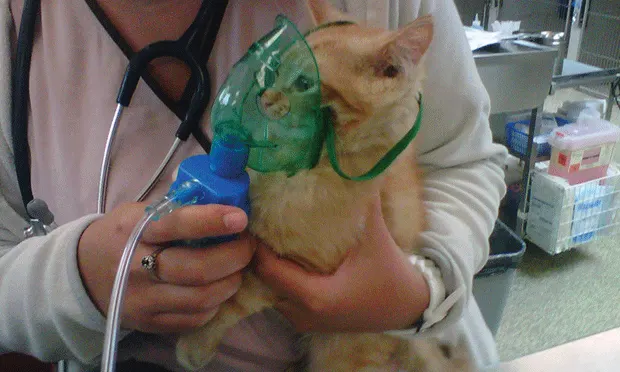
Pulmonary diseases, which are common in dogs and cats, may be infectious, inflammatory, or neoplastic. In the treatment of infectious or inflammatory pulmonary disease, aerosol medication, either as sole therapy or adjunctive to systemic treatment and supportive care, can be beneficial.
To date, most recommendations on inhaled medications are based on opinion or extrapolated from human medicine.
Fast Fact
The term aerosol therapy was introduced in the early 20th century. Since that time, there has been considerable growth in the human field of aerosol therapy.
Aerosol therapy can be an appealing treatment option because it directly channels medication into the respiratory tract. In contrast, some systemic medications fail to adequately reach the source of infection or inflammation, particularly in patients with excessive mucus or established infection in the airway lumen.
Of note, anatomy, physiology, and compliance differ between human and veterinary patients and may influence whether aerosol therapy is successful. For example, although dogs and cats can be trained to tolerate a face mask, they continue to breathe through their noses. Their complex nasal turbinates, however, prevent most aerosolized medication from reaching the lungs, as it is deposited in the nasal cavity instead. Despite nasal breathing and interference of nasal turbinates, there are clear indications for aerosol and inhalation therapy in these patients.
Indications & Complications
Aerosol therapy should be considered as adjunctive therapy in cats and dogs with chronic inflammatory airway disease (eg, feline asthma) and in dogs with aspiration pneumonia or cough from Bordetella bronchiseptica infection. Nebulization is commonly combined with coupage to mobilize secretions.
Considerations
Three types of aerosol generators are used in human medicine: nebulizer, metered-dose inhaler (MDI), and dry-powder inhaler (DPI). DPIs are not used in dogs or cats because of their inability to generate adequate negative pressure on inspiration.
The most common nebulizer is the pneumatic jet, which delivers compressed gas through a jet, causing liquid to break into droplets. A baffle (ie, surface on which large particles fall/deposit) may help make the nebulized particles smaller. Ultrasonic or mesh nebulizers may also be used but are less common.
MDIs create particles by using a pressured propellant called hydrofluoroalkane (HFA). Distribution in the airway depends on particle size, with particles >10 µm removed or trapped in the upper airways, particles of 5 to 10 µm settling in the lower airways, and particles of 1 to 5 µm reaching the lung periphery.
Drug deposition can be a major concern, with large percentages of drug settling in the upper airways. Deposition is reflective of 3 separate mechanisms: inertial impaction, gravitational settling, and diffusion of particles <1 µm. Although drug deposition can be variable, studies using nuclear scanning have established that medication administered by MDIs do reach the lungs, with some of the inhalant likely absorbed systemically.
Successful aerosol therapy depends on properly implementing the required hands-on approach, selecting the appropriate medication, and attaining patient cooperation. Medications should be designed for aerosolization in dogs and cats. Of note, N-acetylcysteine should not be used as an aerosol because of the risk for bronchospasm or airway irritation.
Pet cooperation is essential, especially for patients requiring long-term aerosol therapy; training and positive reinforcement are required. As with all therapies, each treatment plan should be assessed based on individual patient needs. Although inhaled albuterol is an effective bronchodilator, terbutaline (0.01 mg/kg SC) may be preferable to lower feline patient stress in an asthmatic crisis.
Step-by-Step: Nebulization
What You Will Need
Nebulizer (ie, source of compressed air)
Medication
Face mask (optional)
Step 1
Prepare nebulizer with selected product. Children’s nebulizers can be useful and economic in a veterinary setting.

Author Insight
For patients with pneumonia, combine nebulization with physiotherapy (ie, coupage).
Step 2
Nebulize the patient until all liquid has been aerosolized. (A) The nebulizer should be carefully aimed to allow inhalation of the medication, such as using a face mask, rather than (B) placing the nebulizer tube near the patient but not close enough for medication to be inhaled.
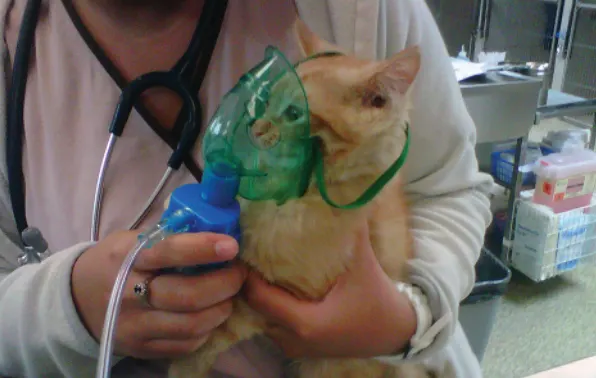
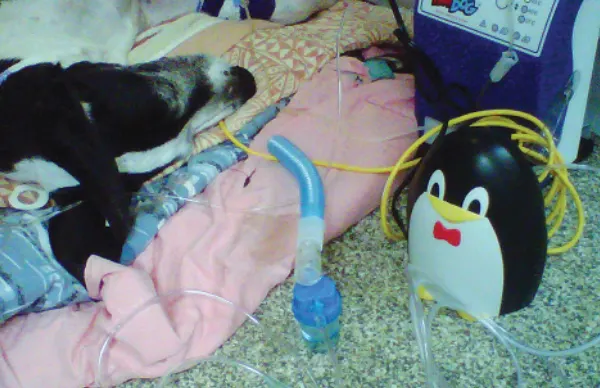
Step 3
Clean and dry all equipment. Sterilization is necessary if the patient has an infectious disease.
Step-by-Step: Metered-Dose Inhalation
What You Will Need
MDI
Face mask
Space chamber (eg, Aerokat, trudellmed.com/animal-health)
Selected drug (eg, albuterol, fluticasone; see Table)
Step 1
Choose the inhalant (see Table). Metered-dose inhalation should be reassessed if the initial patient response to oral glucocorticoids was poor, as inhaled glucocorticoids may be ineffective if systemic glucocorticoids are ineffective. Fluticasone (eg, Flovent) is the most commonly used glucocorticoid in the United States, although other preparations (eg, QVAR) are available. Clients should be informed that inhaled glucocorticoids may be expensive, particularly as compared with oral prednisolone or prednisone.
Table: Commonly Used Inhaled Medications
Author Insight: Restrain the pet comfortably and provide positive reinforcement as needed.
Step 2
Select the face mask and spacer; the latter allows distribution and suspension of the medication. When medication is inhaled by the patient, there is no need to coordinate actuation of the metered dose at the exact inspiration point.

Author Insight
If the MDI has not been used recently, prime it first by shaking gently before actuating 2 to 3 puffs.