Acute Collapse
Elisa M. Mazzaferro, MS, DVM, PhD, DACVECC, Cornell University Veterinary Specialists
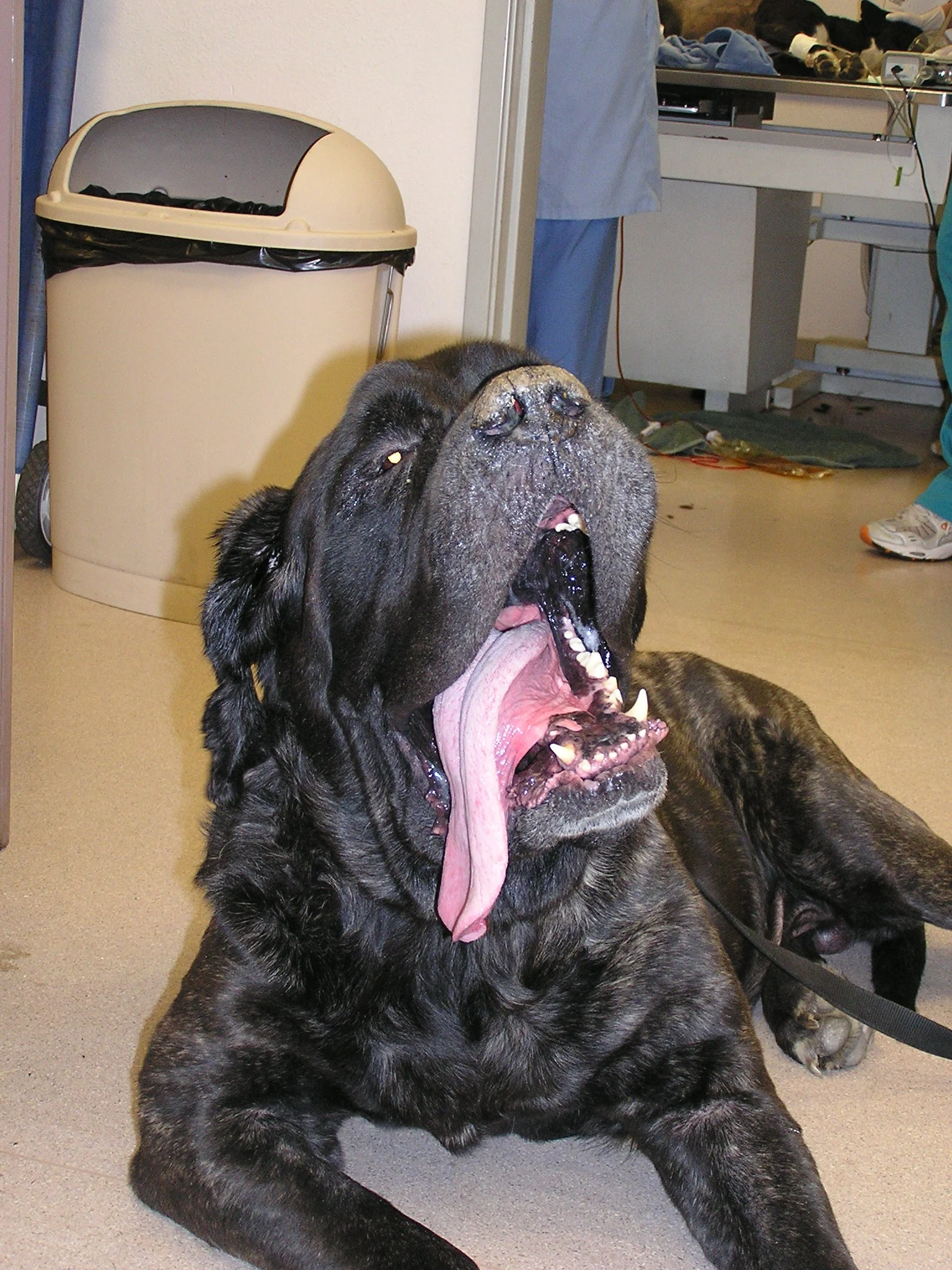
Sherman, a 6-year-old, 78-kg, intact male English mastiff presented to the veterinarian after a 15-kg weight loss and a history of decreased appetite, diarrhea, and sudden reluctance to stand or walk.
History
At the time of presentation, Sherman was mildly hyperthermic (103.2° F), weak, lethargic, and ambulatory only with assistance. His mucous membranes were pale pink and slightly cyanotic with a prolonged capillary refill time (> 2 seconds). Thoracic auscultation revealed irregular heart sounds with no murmurs present. Lung sounds were harsh but were attributed to increased salivation and upper airway noise. A small amount of blood and diarrhea were noted on rectal examination. The prostate was large, nonpainful, and symmetrical. There was an intermittent history of a dry, nonproductive cough. No prior episodes of exercise-induced collapse or collapse at rest were reported.
Initial Diagnostics
A complete blood count revealed mild leukocytosis (15,700 WBC with normal leukogram). Serum biochemistry values were normal. A free-catch urine sample was obtained; urinalysis revealed small numbers of cocci with no evidence of pyuria. Next, abdominal ultrasonography showed prostatomegaly. A presumptive diagnosis of prostatitis was made. Sherman was referred to a specialist for further medical care.
Physical Examination
At the time of presentation to the referral hospital, Sherman was weak and lethargic. He had a sporadically irregular heartbeat and pulse deficits, was thin (body condition score 2/5), and had a poor hair coat with generalized superficial pyoderma. Mucous membranes were pale pink and slightly cyanotic. Lung sounds were harsh with crackles in the mid to dorsal lung fields. He was ambulatory only with assistance. Cranial nerve examination was normal. The patient was weak but was able to stand and walk with assistance. Spinal reflexes, withdrawal, and conscious proprioception were all normal.
Further Diagnostics
Sherman was normotensive (148 mm Hg systolic/70 mm Hg diastolic; mean arterial pressure 107 mm Hg). ECG revealed the rhythm shown in Figure 1. Thoracic radiographs showed marked cardiomegaly without evidence of pulmonary edema. Echocardiography revealed biventricular and biatrial enlargement with decreased fractional shortening (19%) (Figure 2).

FIGURE 1 Lead II electrocardiogram (paper speed 25 mm/sec) performed at the time of presentation

FIGURE 2 M-mode echocardiogram denoting extremely poor fractional shortening. Note the relatively small change in ventricular internal diameter during systole and diastole.
Ask Yourself...
In a collapsed patient, what diagnostic tests should be performed first?
What is the rhythm shown in Figure 1?
Should Sherman be treated for prostatitis?
What is his prognosis?
Diagnosis: Dilated cardiomyopathy
Based on Sherman's signalment, history, presenting clinical signs, and echocardiogram findings, a diagnosis of dilated cardiomyopathy with systolic heart failure was made. A nasopharyngeal oxygen catheter was placed, and supplemental oxygen was administered (100 ml/kg/min). The ideal treatment for dilated cardiomyopathy is directed at increasing cardiac contractility and decreasing heart rate. Rhythm control with biphasic electrocardioversion has also been described, but the owners declined this therapy.
Digoxin (0.325 mg PO Q 12 H) was prescribed as a positive inotrope and negative chronotrope and is considered one of the mainstays of therapy for DCM. More recently, the use of pimobendan, a positive inotrope and venoarteriolar dilating drug, has been associated with improved survival and quality of life in Doberman pinchers and cocker spaniels with DCM.1 Sherman's clinical condition improved over the next 2 days of therapy, and he was discharged from the hospital with the following oral medica-tions: enalapril maleate (20 mg PO Q 12 H), furo-semide (25 mg PO Q 12 H), digoxin (0.375 mg PO Q 12 H), and diltiazem (45 mg PO Q 8 H).2
Reevaluations of the ECG, digoxin levels, and echocardiogram were done 2 weeks after the initial presentation and revealed continued atrial fibrillation with slowing of the ventricular rate, normotension (BP 130 mm Hg SBP; 65 mmHg DBP), and improved fractional shortening (increased to 29%). Sherman's owner reported that he was active and alert and had a good appetite. He had gained 4 kg in the 2 weeks since the diagnosis and initiation of treatment. Sherman survived for 4 months after the initial diagnosis was made.
Did You Answer ...
ECG and blood pressure monitoring should always be considered as first-line diagnostics in any animal with a history of acute collapse and clinical signs of inadequate cardiac output or inadequate tissue perfusion. Sherman was weak and collapsed because of low cardiac output. Cardiac output is a function of both heart rate and stroke volume. Stroke volume is a function of cardiac preload, afterload, and contractility. The hypotension with end-organ insufficiency (in this case manifested by diarrhea) can be attributed to poor cardiac contractile function and rapid heart rate impairing adequate diastolic filling, leading to decreased cardiac preload.
The rhythm is atrial fibrillation, which is common in dogs with DCM. Note the sporadically irregular QRS complexes and fibrillation waves. Atrial fibrillation can be controlled with such negative chronotropic drugs as digoxin, beta-blockers (propranolol, atenolol), and calcium-channel blockers (diltiazem). Rhythm can be controlled with biphasic electrocardioversion, although this therapy was declined. Calcium-channel and beta-adrenergic blockers must be used with caution, as both can be negative inotropes and contribute to inadequate cardiac contractility in cases of DCM.
No. Prostatomegaly with no evidence of fever, prostatic pain, or pyuria is a benign condition in intact male dogs, although it can occasionally have adverse consequences. Sherman's poor body condition, weakness, and collapse were associated with inadequate cardiac output secondary to poor cardiac contractility and atrial fibrillation. In this case, the finding of prostatomegaly on abdominal ultrasonography was incidental. The few cocci without evidence of white blood cells in the urine sediment was associated with this patient's dermatologic condition and a free-catch urine sample, not prostatitis.
In large-breed dogs, such as English mastiffs, lone atrial fibrillation can occur without underlying heart disease. Median survival time after the development of atrial fibrillation and clinical signs of heart failure is typically 6 to 12 months after a diagnosis is made. The presence of atrial fibrillation with decreased fractional shortening are negative prognostic indicators, and may be associated with sudden death.
Treatment at a Glance
For acute care
Place a nasopharyngeal oxygen catheter with supplemental oxygen (100 ml/kg/min).
Digoxin (0.325 mg PO Q 12 H as a positive inotrope and negative chronotrope); pimobendan, a positive inotrope and venoarteriolar dilating drug, has been associated with improved survival and quality of life in Doberman pinchers and cocker spaniels with DCM.
Controlling rhythm with biphasic electrocardioversion has also been described.
Discharge with
Enalapril maleate (0.5 mg/kg PO Q 12 H)
Furosemide (2.2-4.4 mg/kg PO Q 12 H)
Digoxin (0.005-0.01 mg/kg PO Q 12 H, maximum dose 0.375 mg Q 12 H)
Diltiazem (10 mg/kg PO Q 12 H)