Top 5 Dental Emergencies
Judy Rochette, DVM, FAVD, DAVDC, West Coast Veterinary Dental Services
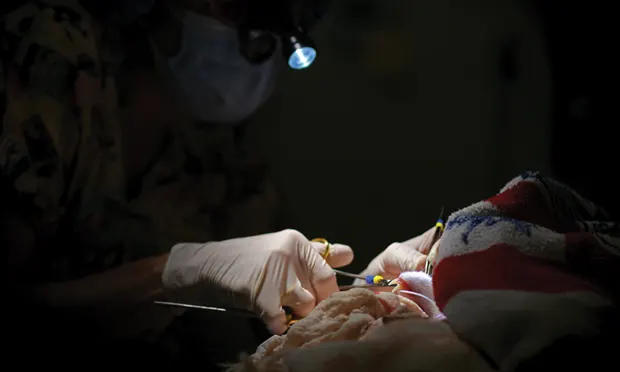
Emergency orodental presentations requiring immediate attention tend to involve, or lead to, dysfunction and pain. Identification of pathology may be challenging in an awake or distressed animal; analgesics and radiographs can be invaluable.
1. Orodental Trauma: Hard Tissue
The most common emergency associated with the oral cavity is an insult that results in fractures with pain, hemorrhage, loss of function, and risk for infection.1 High-energy impact, pathologic conditions (eg, neoplasia), injury from another animal, and self-generated trauma can all result in harm to the facial bones and/or the teeth. Mandibular fracture, symphyseal separation, traumatic clefting of the hard palate, and temporomandibular joint dislocation are among the most common injuries and can result in facial asymmetry, deviation of the jaws, epistaxis, visible soft-tissue tearing, malocclusion, and visible dental fractures (Figure 1).


Fractures caused by orodental trauma are usually compound, with soft-tissue tearing and hemorrhage, and result in malocclusion (A). An intraoral resin splint is an effective, minimally invasive treatment technique (B).
Initial stabilization of the patient should include analgesics and antibiotics, as almost all bony fractures involving the oral cavity are compound and therefore at risk for infection. The author prefers buprenorphine or hydromorphone for analgesia and clindamycin for antibiotic coverage, as these all come in an injectable form. Unsedated skull radiographs can give an initial overview of possible damage, but intraoral radiographs are necessary to accurately assess orodental fractures. Sedation and/or anesthesia may be contraindicated until the initial head, brain, or shock trauma is controlled.
To prevent further trauma, immobilization of the fractured area (eg, with a tape muzzle) should be incorporated as indicated. Nutritional support may be needed until definitive treatment can be safely accomplished. Intraoral resin splints, interdental wiring, interfragmentary wiring, and mini-plates are all possible treatment options.



Orodental trauma involving soft tissue requires hemostasis (A), debridement (B), and closure (C) but often results in rapid return to function. Photos courtesy of Lara E. Bartl, DVM, DABVP
2. Orodental Trauma: Soft Tissue
Trauma that damages orodental soft tissue tends to damage the tongue, pharynx, soft palate, or oral mucosa (Figure 2). Impalement, foreign bodies, and topical irritants are possible sources of harm. Hemostasis, wound debridement, and closure should be completed, and mastication, deglutition, and respiratory function should be verified. Distant sites that may also have been affected (eg, retropharyngeal area, lungs, liver) should be monitored. In general, soft-tissue injuries treated appropriately tend to heal well because of the excellent blood supply to the head and neck.
3. Tooth Fracture, Avulsion, or Intrusion
All fractured teeth with pulp exposure will be painful and will allow bacterial ingress leading to infection and eventual loss of the tooth. Any tooth with pulp exposure requires endodontic treatment or extraction. Allowing a fractured tooth to go untreated is inappropriate.

When forces overwhelm the support apparatus, soft-tissue tearing and visible displacement of the tooth can be seen.
A force that overwhelms the attachment apparatus of the tooth will cause displacement of the tooth from its normal position in the socket (Figure 3). Displacement can involve movement within the socket but with some persisting attachment of supporting tissues (luxation) or a complete loss of the tooth from the socket (avulsion). Intrusion involves displacement of the tooth through the apex of the socket. Intrusion occurs most commonly to the maxillary canine teeth, with the tooth coming to rest in the nasal passages. Maintaining and restoring the tooth to function can be achieved if the tooth is kept moist, quickly returned to its correct position within the socket, and stabilized until the supporting apparatus can heal. Displacement causes loss of the tooth’s blood supply; therefore, endodontic therapy is necessary.
4. Inability to Open or Close the Mouth
Trigeminal nerve dysfunction may result in a flaccid, nonpainful inability to close the mouth. Trigeminal injury may be perceived as idiopathic. However, inflammation, direct trauma to the nerve from stretching or impact, and, in rare cases, neoplasia, can induce flaccid paralysis. Passage of time and/or anti-inflammatories, combined with assisted feeding, will usually result in resolution. Imaging and biopsy may be needed to rule out neoplasia, which, by its nature, has a more guarded prognosis. Rarely, rabies may present with flaccid paralysis of the face; therefore, in endemic areas, vaccine status of the animal should be verified.
Interference between the dorsal coronoid process and the zygomatic arch will also hinder closure of the mouth, but this tends to result in a distressed, likely painful, patient. Sedation or full anesthesia may be necessary to return the mandible to its proper position. The animal is usually fully functional immediately after treatment, but surgery to remove the dorsal portion of the coronoid process and the central zygomatic arch may be needed if the mandible cannot be replaced or if the problem recurs. Traumatic fractures, dislocation of the temporomandibular joint, or displacement of a tooth can also inhibit mouth closure by tooth-on-tooth interference or tooth-on-soft-tissue contact. Treatment is correction of the underlying cause.

Periorbital swelling, prolapsed nictitans, and epiphora are secondary to retrobulbar cellulitis and/or abscessation.
An acute inability to open the mouth can be secondary to masticatory muscle myositis, retrobulbar cellulitis and/or abscessation, or tetanus. Masticatory muscle myositis may present with swollen temporal (and occasionally masseter) muscles, pain, and fever. Confirmation is via biopsy of muscle bodies. Initial treatment is with immunosuppressive doses of steroids. Retrobulbar cellulitis or abscess may produce periorbital swelling and/or exophthalmos of the affected eye. (Figure 4). The patient can open its mouth but resists because of the acute pain such movement will cause. Establishing drainage, anti-inflammatories, and antibiotics is often sufficient to resolve the problem. Occasionally, a foreign body will need to be located and removed in order to achieve permanent resolution. Tetanus is rare in cats and dogs and more common in guinea pigs and horses.2 Progression of clinical signs (eg, drooling, risus sardonicus, muscle spasms, respiratory paralysis) after infection with Clostridium tetani bacteria can be rapid. Treatment may involve antibiotics, antiserum, nursing and ventilatory support, and muscle relaxants. Retrobulbar neoplasia may occasionally present with acute clinical signs.3 Advanced imaging may be needed to diagnose and confirm this condition. Prognosis is guarded, as invasion into periorbital structures can occur before clinical signs present.
5. Anorexic Small Mammal

A lagomorph with dental disease with secondary ocular and nasal discharge.
Dental disease with an inability to masticate should be on the differential list for any anorexic small mammal.An anorexic lagomorph (Figure 5) or rodent is at serious risk for ileus, which can be life-threatening.4 Owners may perceive the onset of illness as acute if they are not aware of a change in food preferences, decreased intake, and/or decreased fecal output. Drooling, weight loss, proptosis of the eyes, facial abscessation, and lethargy are common signs.
Stabilization prior to treatment may be necessary and could include feeding, fluids, gut motility modifiers, analgesics, and thermal support. An intraoral examination, combined with intraoral and/or extraoral radiographs, is necessary to accurately locate the source of the problem. Treatment involves returning the occlusal arcades to more normal anatomic lengths, extractions as needed, and treatment of any abscesses. Postoperative care must support the patient until it is able to maintain bodily functions on its own.
Conclusion
True emergency situations may occur less frequently than in other disciplines, but orodental emergencies must be properly assessed so that correct treatment can be instituted. Return to function needs to be timely for patient survival.