Struvite Urolithiasis
Gregory F. Grauer, DVM, MS, DACVIM (SAIM), Kansas State University
You have asked…
How can I treat and manage struvite urolithiasis in cats and dogs?
The expert says…
Struvite uroliths in dogs and cats are commonly composed of struvite (ie, magnesium ammonium phosphate), although they may also contain calcium phosphate (hydroxyapatite) or calcium carbonate.
Owing to high dietary intake of protein and minerals, canine and feline urine is frequently supersaturated with respect to struvite; however, in dogs, urinary tract infection (UTI) is an important predisposing factor to formation of uroliths. Staphylococcus, Proteus, Enterococcus, and Mycoplasma spp are commonly associated pathogens because they produce urease and can split urea into ammonia and carbon dioxide.
Because of their high association with UTIs, struvite uroliths are more common in female dogs, accounting for more than 80% of uroliths in this population.
Hydroxyl and ammonium ions formed by ammonia hydrolysis can decrease hydrogen ion concentrations in urine, resulting in alkaline urine and decreased struvite solubility. Urea hydrolysis can also increase urine concentrations of ammonium and phosphate ions, which can increase urine supersaturation. In addition, high urine ammonia concentrations can damage glycosaminoglycans that help prevent bacteria from adhering to urinary mucosa. Finally, bacterial cystitis increases the amount of organic debris available as a surface for crystallization.
Because of their high association with UTI (Figure 1), struvite uroliths are more common in female dogs, accounting for more than 80% of uroliths in this population.1 Similarly, uroliths in dogs younger than 1 year of age are usually struvite and typically associated with UTI. Of 800 uroliths retrieved from dogs less than 1 year of age and subsequently analyzed at the University of Minnesota Urolith Center, 56% were struvite and 23% were purine.2
Figure 1A. Right lateral radiograph of a spayed long-haired dachshund (7 years of age) with UTI and multiple struvite urocystoliths; 100% struvite uroliths.
In cats, uroliths typically develop in the absence of UTI (Figure 2). Greater urine-concentrating ability and urine supersaturation may be partially responsible for urolith formation in cats and dogs without UTIs. In addition, formation of sterile struvite uroliths may be facilitated if urine pH is consistently elevated (eg, because of drugs, diet, renal tubular disorder) enough to increase the activity product of struvite to induce precipitation.
Figure 2B. 100% struvite uroliths (scale: 1 division = 1 mm).
Struvite uroliths may occur in any breed, although the miniature schnauzer, miniature poodle, bichon frise, and cocker spaniel are commonly affected. The high prevalence of struvite uroliths in the cocker spaniel suggests familial predisposition in this breed.3
Best Methods: Treating Struvite Urolithiasis
Medical dissolution of struvite uroliths can be effective, although the choice between surgical removal versus medical dissolution is not always clear. Disadvantages of surgery include need for anesthesia, potential surgical complications, and possibility of incomplete urolith removal; advantages include the ability to definitively identify urolith type, correct concurrent or predisposing anatomic abnormalities (eg, urachal remnants, urinary bladder polyps), and obtain samples of urinary bladder mucosa for bacterial culture if urine culture yielded no growth.
Medical treatment can lower the concentration of calculogenic minerals in urine, increase mineral solubility in urine, and increase urine volume. The major disadvantage of medical treatment is the need for considerable owner compliance for several weeks to months. The cost of medical dissolution is usually less than that of surgery, despite the frequent need for multiple follow-up urinalyses, bacterial cultures, and imaging studies (radiography and/or ultrasonography). Urethral obstruction during medical dissolution is uncommon; however, patients with struvite urolith–induced obstructive uropathy cannot be treated medically. In addition to medical dissolution, voiding urohydropropulsion or catheter retrieval can be used to nonsurgically remove cystouroliths in some patients. Lithotripsy, available at referral centers, has also been used as a successful treatment for nephroliths and, less commonly, ureteroliths in dogs.
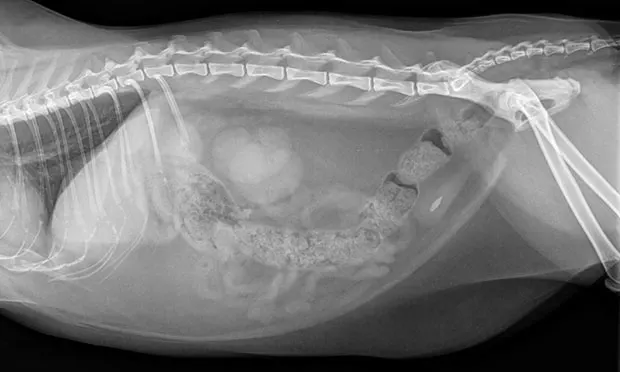
Figure 2A. Lateral radiograph of a spayed domestic short-haired cat (6 years of age) showing a single struvite urocystolith; a 100% struvite urolith.
Figure 2B. A 100% struvite urolith was removed (scale: 1 division = 1 mm).
General preventive measures include diuresis induction and UTI eradication. Diuresis is important because it lowers urine specific gravity (USG) and urinary concentration of calculogenic minerals. Feeding canned food can help increase water intake. In general, maintaining USG below 1.020 (dogs) or 1.035 (cats) is ideal. Dogs should be allowed frequent voiding opportunities to facilitate washout of bacteria and crystalline aggregates. Urine sediment and pH should be monitored routinely and UTIs treated promptly, based on bacterial culture and sensitivity results.
In dogs, struvite uroliths can usually be dissolved by feeding a struvite dissolution diet (eg, Hill’s Prescription Diet s/d Canine Dissolution, Royal Canin Veterinary Diet Urinary SO). An average of 8 to 10 weeks (range, 2 weeks–7 months) is needed to dissolve the uroliths. The rate at which uroliths dissolve is proportional to the surface area of the urolith exposed to undersaturated urine and the presence or absence of UTI (sterile struvite uroliths dissolve more rapidly than those associated with UTI).2 Dissolution diets should not be fed routinely for maintenance and should not be used in pregnant, lactating, or growing patients or after surgery (as restricted dietary protein may compromise wound healing). Because of its high salt content, such diets should not be fed to dogs with congestive heart failure, hypertension, or nephrotic syndrome. In miniature schnauzers, the high fat content of these diets may exacerbate any lipid abnormalities and increase the risk for pancreatitis.
A dissolution diet should be fed for a minimum of 30 days after calculi are no longer visible on radiographs. Struvite dissolution diets are not effective with nonstruvite uroliths, if UTI persists, or if the patient is fed anything in addition to the dissolution diet.
Elimination of any bacterial UTI is an essential part of medical treatment. If infection was present when treatment started, antibiotic therapy should be continued throughout treatment, as viable bacteria may be liberated from dissolving uroliths. Antibiotic selection should be based on urine culture and sensitivity findings. In patients with severe or persistent UTI caused by urease-producing bacteria, the urease inhibitor acetohydroxamic acid (Lithostat, lithostat.com) may be added but is rarely needed; at a dose of 12.5 mg/kg PO q12h, it may help dissolve struvite uroliths resistant to antibiotic and dietary treatment. Adjunctive treatment with urinary acidifiers with the struvite dissolution diet is usually not recommended. The most common causes of alkaline urine during dietary treatment are persistent bacterial infection and lack of dietary compliance. Medical treatment of sterile struvite uroliths does not require antibiotic treatment.
Approximately 45% of uroliths in cats consist either entirely or predominantly of struvite, and most feline struvite uroliths form in sterile urine.4 When bacterial infection is present, the most common organism is a urease-producing Staphylococcus spp.
Effective feline dissolution diets are currently available and take an average of 3 to 4 weeks to dissolve sterile struvite uroliths versus 2.5 months for struvite uroliths associated with urease-producing bacterial infection.2 Antibiotic treatment in cats with struvite urolithiasis and concurrent bacterial UTI should be based on urine culture and sensitivity results and continued throughout dissolution. The dissolution diet should be fed for 30 days beyond the point when uroliths are no longer visible on radiographs.
Best Practices: Preventing Recurrence
A diet moderately restricted in protein, magnesium, calcium, and phosphorus content that results in acidic urine is a good option in dogs.
Measures to prevent struvite urolith recurrence include preventing and controlling UTI, maintaining acidic urine, and decreasing dietary intake of calculogenic minerals (see Feline Struvite Prevention Diets). A diet moderately restricted in protein, magnesium, calcium, and phosphorus content that results in acidic urine is a good option in dogs. In dogs with recurrent UTI, predisposing abnormalities (eg, abnormal vulvar anatomy, urethral sphincter mechanism incompetence) should be identified and corrected. Otherwise, silent hyperadrenocorticism may also result in recurrent UTI. Routine urinalyses should be performed q2–4mo in subclinical patients and follow-up urine cultures performed in patients with clinical signs or urine sediment changes compatible with lower urinary tract inflammation. Struvite prevention diets are usually ineffective in the face of subsequent UTIs.
UTI = urinary tract infection, USG = urine specific gravity